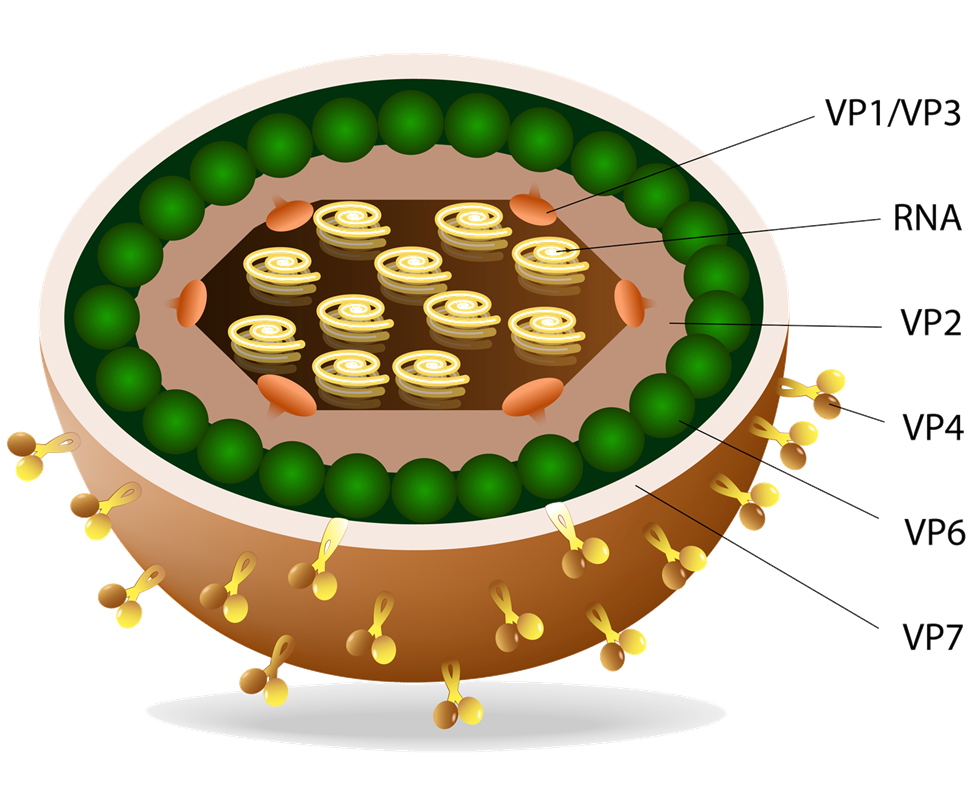
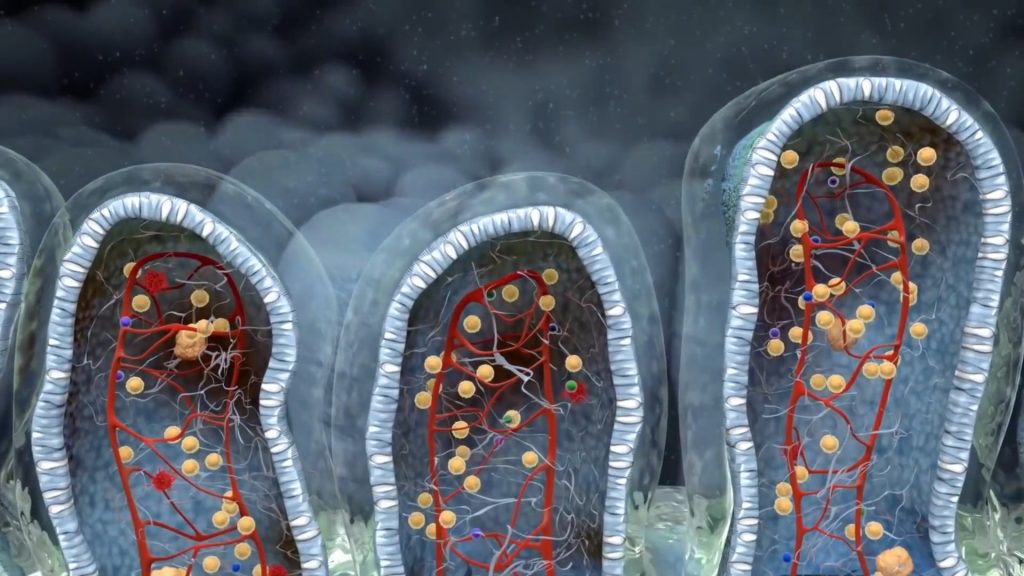
Post cholecystectomy IBS
IBS patients who presented with bile diarrhea after gallbladder removal or their symptoms exaggerated after the operation. IBS may manifest directly after the removal up to 7 years later
Number of cases
Mean age
Rate of success
Treatment duration
Most common symptom
Most common culprit
The spectrum of the symptoms is similar, not only for the 339 cases mentioned above, but in hundreds more when it comes to gallbladder removal. It is the physiological changes that takes place inside our GI system, and some extra-bowel organs, that most of the times give rise to the classic post-cholecystectomy IBS. It is highly treatable with the highest percentage of content patients. Nevertheless, there are several behavioral and nutritional guidelines that should be followed, even after treatment has finished. Besides, our gallbladder has evolved several hundred thousand years coexisting and communicating directly or indirectly with many other organs. So, inevitably, its removal changes this communication and alters most of the digestion processes. Oddly, several times, some symptoms already existed before cholecystectomy, although usually in a milder form. This means that gallbladder stones were not the problem in the first place.
Alkaline gastritis
The constant infux of alkaline bile into the highly acidic gastric environment leads to alkaline gastritis
Bowel pH
The bowel-liver circulation of bile is gradually compromized, leading to the alkalization of the large intestinal environment
Dysbiosis
The gradual shift of large bowel physicochemical properties leads to alterations of the microbial ecology, usually towards fermentative populations
Fat malabsorption
After the operation, bile is not regulated by gallbladder contractions, thereby less bile is available at a given time for fat absorption, leading to metabolic alterations
Gastric acidity
The compensating mechanism that dictates the amount of gastric juice is partially regulated by gallbladder contractions, leading to gradual hypochlorrhydria (reduced gastric acidity)
Pancreatic output
After cholecystectomy, the pancreas receives less signal for pancreatic enzyme preparation, leading to gradual decline in its output capacity. Besides, exocrine pancreatic insufficiency is diagnosed in about 25% of patients that have undergone gallbladder removal
Athina was a 46 years old mother of 2 boys and visited my office on June 2016. Being a lawyer means that she is always in crowded places and most of the times she could not leave in order to visit the bathroom. She had removed her gallbladder soon after she stopped breastfeeding her second child, due to stone formation. She had already done every endoscopic test exists and already tried several drugs, mostly spasmolytics. Of course nothing worked, since the problem is not the bowel moving too fast, but the substances that flow into her large bowel and make it want to get rid of them.
For example, if bile (an alkaline substance) goes into the colon (acidic environment), the bowel cannot tolerate it. So it starts throwing water from the wall in order to get rid of it, thus giving rise to diarrhea. This may happen several times within a day since bile keeps flowing down. And it is not the only way gallbladder removal may induce bowel problems.
Everyday habits that do not nourish the microbial ecology lead to longterm metabolic and immune perturbations
Intesne antibiotic use may induce physicochemical alterations of the mucosal surface as well as abrupt dysbiosis
The removal of a very important organ alters the physiology of digestion, makes the intestinal surfaces more alkaline and leads to the post-cholecystectomy syndrome
Due to the inappropiate fiber fermentation, she avoided vegetable and grain consumption leading to the shrinking and worsening of microbiome diversity
According to Athina’s medical history and her major complaints I asked her to perform several stool and blood tests. First I wanted to address the urgency to run to the toilet. If we could limit this symptom then we would have time to address the others. Generally, patients’ psychology is crucial in order for the treatment to work better and to achieve maximum compliance. That’s why first we need to take care of some symptoms, even if it means that we just treat them and not cure them. In this context, I asked her to perform a series of tests, including a special stool test, and several blood absorption markers, and to keep an initial diary in order to correlate foods with symptom patterns.
The presence of a highly alkaline molecule inside the colon in larger, than normal amounts, increases the urge of the colon to get rid of it, thus contracting faster, leading to the feeling of urgency
Diarrhea is an evolutionary mechanism that protects us from potentially dangerous or infectious particles inside our large intestine. Bile or indigested particles may set this mechanism in action
The feeking of incompleteness after defecation is usually both neurological and secretory. This symptom usually accompanies the aforementioned urgency as they share common pathways
Having constanly less bile than needed leads to fatty vitamin and nutrient malabsorption. Gradually, this nutrient loss lead to fatigue and other functional symptoms
Athina has been having daily episodes of bile diarrhea resulting from the excess bile that escaped her terminal ileum and entered her colon. Her colon, in turn, could not manage the extra bile so it started secreting water and mucus in order to get rid of it. This is the definition of bile diarrhea which includes soft stool, not just watery. Bloating and flatulence resulted from abnormal degradation and fermentation of fibers and starch that reached her colon. This explains her abnormal gas distribution, and thus her bloating. Finally, her fatigue and her extra-intestinal symptoms could be explained by the excess histamine and mycotoxins produced by Klebsiella and Candida, respectively.
Bile leak
Bile leaking into the colon produces massive water, electrolyte and mucus excretion, and thus softer stool up to diarrhea. This is also an urgent signal for defecation.
Klebsiella pneumoniae
Klebsiella is a potent fermenter of starch and histamine producer. Loose stool, bloating and vagotonia may be symptoms of its overgrowth

Candida albicans
Candida is a potent fermenter of sugars and produces large amounts of mycotoxin which may aggravate diarrhea.

Probiotic sterility
Probiotic sterility leads to abnormal fermentation of starch, sugars and fiber. Bloating and gas are main symptoms while limited production of vitamins like biotin and vitamin K may contribute to fatigue
While there were four findings needed to be carefully addressed, bile binding is crucial in order all the other components to take effect. In addition, specialized probiotics are needed in this case, since bile changes the physicochemical properties of the gut epithelium. Probiotics are microorganisms that live in distinct areas of our gut lining and each strain has different environmental requirements to thrive and survive. This is why reinoculation of new colonies is a very difficult task and the patient has to be very compliant in order to achieve recovery. Even if someone takes tons of probiotics, if the pH of the gut is not correct, if the width of the mucosal layer is not sufficient or if there are competing bacteria nearby, the colonization will fail and all the patient is going to get is intensified symptoms.

After Athina started the treatment I asked her to call me after one week. She was very happy because finally after several months she could see formed stools and her bloating was at least 50% better. After 40 days we spoke and the conversation was very short since she had nothing to report to me. Everything was going very well, she had one or two defecations daily, her stools were formed and consistent and she had also gained 2 kg.
This case represents a great number of Irritable Bowel Syndrome patients that have removed their gallbladder. This type of surgery alters many of the physiologic processes that take place in our gut and produce different symptoms that may differ in the time of initiation, the severity and sometimes may give rise to different IBS subtypes. For example, cholecystectomy can sometimes lead to constipation predominant IBS, which is much more difficult to treat than diarrhea predominant IBS. Usually, these patients seek a more advanced diagnosis several years after the onset of the symptoms, something that makes treatment more difficult; the reason being that the longer bile destroys flora, mucosal lining and the colonic environment the harder is to restore it.
- Gallbladder removal modulates many biochemical, hormonal and structural properties of the digestive process
- The change of pH values in both the large intestine and the stomach predisposes for inflammation, colitis and gastritis respectively
- The time needed after cholecystectomy in order for a patient to experience IBS symptoms depends on the previous state of gut health and previous lifestyle choices
- Bloating or flatulence after fiber consumption is an indirect effect of cholecystectomy. Alkaline bile changes the environment where normal acidic commensal bacteria would normally thrive
- Urgency after cholecystectomy is the physiologic way our gut nervous system possesses to inform us that there is something inside that must be eliminated fast

With a background in Chemistry and Biochemistry from the National and Kapodistrian University of Athens, Theodoros brings a wealth of knowledge in functional medicine and advanced treatments to his role. He possesses exceptional skills in analysis, pattern recognition, diagnostic translation, and storytelling. He is also FMU certified in Functional Medicine and has received training in advanced treatments from the Saisei Mirai Clinic in Japan.